Longitudinal, representative studies on mental health consequences of the COVID-19 pandemic
This regularly updated table presents studies investigating mental health burden of the COVID-19 pandemic in the general population as well as in other target groups. The studies presented in the table were selected according to the following criteria:
All studies are required to
report a measure of mental health assessed with a validated measurement tool;
provide a longitudinal study design (several assessments of the same individuals);
provide a comparison between values assessed before and after the beginning of the COVID-19 pandemic;
provide a sample size > 1000;
Studies in the general population are required to provide a representative sample of the population in the respective country.
These selection criteria are employed to ensure a high quality of the presented data.
The last two columns present the reported statistics for the change between values assessed before and during the pandemic and the direction of this change (increase, decrease, or stability of the respective variable) in a simplified way.
Update: March 25, 2021
Longitudinal studies COVID-19 pandemic
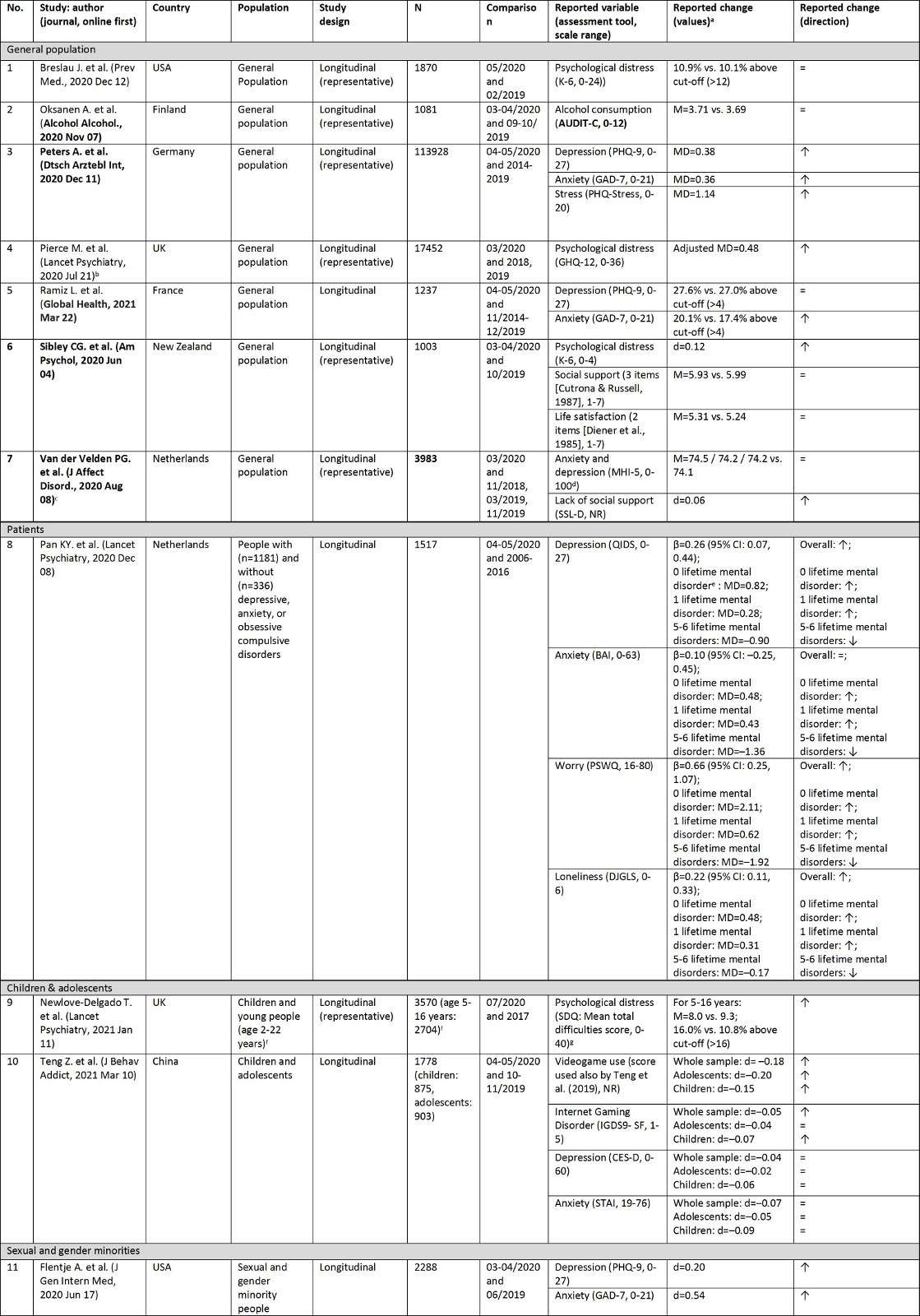
Notes
a first value refers to assessment before the COVID-19 pandemic, second value to the assessment during the COVID-19 pandemic.
b identical study reported by Cheng Z. et al., Daly M. et al., Niedzwiedz CL. et al., Proto E. et al.
c identical study reported by van der Velden PG. et al. 2
d higher values indicate less symptoms of anxiety and depression.
e England: 11 946 696, Northern Ireland, Scotland and Wales: 2 263 811.
f per 100 000 person-months, compared to the estimated expected rates in the pre-COVID-19 comparison period (Jan 1, 2010–Feb 29, 2020); data on referrals to mental health services only available for NI, S, and W.
g pre-existing mental disorders, refers to all reported data on lifetime mental disorders in this study.
h in 2017 n=2589 with age between 5 and 16 years; comparison between 2020 and 2017 only available for age 5-16 years.
i based on information from the parent interview.
↑ increase; ↓ decrease; = no change.
95% CI: 95% confidence interval; d (Cohen’s d): effect size (0.2-small effect, 0.5-moderate effect, 0.8-large effect); E: England; GP: general practitioner; M: mean; MD: mean difference; N: sample size; NI: Northern Ireland; NR: not reported; S: Scotland; vs.: versus; W: Wales
Abbreviations (assessment tools):
AUDIT-C: Alcohol Use Disorders Identification Test; BAI: Beck Anxiety Inventory; DJGLS: De Jong Gierveld Loneliness Scale; GAD-7: Generalized Anxiety Disorder-7; GHQ-12: General Health Questionnaire-12; K-6: Kessler-6 Distress-Scale; MHI-5: Mental Health Index-5; PHQ: Patient Health Questionnaire; PSWQ: Penn State Worry Questionnaire; QIDS: Quick Inventory of Depressive Symptoms; SDQ: Strengths & Difficulties Questionnaire; SSL-D: Social Support List - Discrepancy
References
Breslau J. et al.
Breslau J, Finucane ML, Locker AR, Baird M, Roth E, Collins RL. A longitudinal study of psychological distress in the United States before and during the COVID-19 pandemic. Prev Med. 2020 Dec 12:106362. doi: 10.1016/j.ypmed.2020.106362. Epub ahead of print. Link to PubMed
Cheng Z. et al.
Cheng Z, Mendolia S, Paloyo AR, Savage DA, Tani M. Working parents, financial insecurity, and childcare: mental health in the time of COVID-19 in the UK. Rev Econ Househ. 2021 Jan 12:1-22. doi: 10.1007/s11150-020-09538-3. Epub ahead of print. Link to PubMed
Daly M. et al.
Daly M, Sutin AR, Robinson E. Longitudinal changes in mental health and the COVID-19 pandemic: evidence from the UK Household Longitudinal Study. Psychol Med. 2020 Nov 13:1-10. doi: 10.1017/S0033291720004432. Epub ahead of print. Link to PubMed
Flentje A. et al.
Flentje A, Obedin-Maliver J, Lubensky ME, Dastur Z, Neilands T, Lunn MT. Depression and Anxiety Changes Among Sexual and Gender Minority People Coinciding with Onset of COVID-19 Pandemic. J Gen Intern Med. 2020: 35, 2788–2790. https://doi.org/10.1007/s11606-020-05970-4. Link to PubMed
Newlove-Delgado T. et al.
Newlove-Delgado T, McManus S, Sadler K, Thandi S, Vizard T, Cartwright C, Ford T; Mental Health of Children and Young People group. Child mental health in England before and during the COVID-19 lockdown. Lancet Psychiatry. 2021 Jan 11:S2215-0366(20)30570-8. doi: 10.1016/S2215-0366(20)30570-8. Epub ahead of print. PMID: 33444548. Link to Pubmed Link to NHS.uk
Niedzwiedz CL. et al.
Niedzwiedz CL, Green MJ, Benzeval M, Campbell D, Craig P, Demou E, Leyland A, Pearce A, Thomson R, Whitley E, Katikireddi SV. Mental health and health behaviours before and during the initial phase of the COVID-19 lockdown: longitudinal analyses of the UK Household Longitudinal Study. J Epidemiol Community Health. 2020 Sep 25:jech-2020-215060. doi: 10.1136/jech-2020-215060. Epub ahead of print. Link to PubMed
Oksanen A. et al.
Oksanen A, Savolainen I, Savela N, Oksa R. Psychological Stressors Predicting Increased Drinking During the COVID-19 Crisis: A Longitudinal National Survey Study of Workers in Finland. Alcohol Alcohol. 2020 Nov 7:agaa124. doi: 10.1093/alcalc/agaa124. Epub ahead of print. PMID: 33160284. Link to PubMed
Pan KY. et al.
Pan KY, Kok AA, Eikelenboom M, Horsfall M, Jörg F, Luteijn RA, Rhebergen D, van Oppen P, Giltay EJ, Penninx BW. The mental health impact of the COVID-19 pandemic on people with and without depressive, anxiety, or obsessive-compulsive disorders: a longitudinal study of three Dutch case-control cohorts. Lancet Psychiatry. 2020 Dec 8; DOI: https://doi.org/10.1016/S2215-0366(20)30491-0 Link to PubMed
Peters A. et al.
Peters A et al. The impact of the COVID-19 pandemic on self-reported health—early evidence from the German National Cohort. Dtsch Arztebl Int 2020; 117: 861–7. DOI: 10.3238/arztebl.2020.0861 Link to PubMed
Pierce M. et al.
Pierce M, Hope H, Ford T, Hatch S, Hotopf M, John A, Kontopantelis E, Webb R, Wessely S, McManus S, Abel KM. Mental health before and during the COVID-19 pandemic: a longitudinal probability sample survey of the UK population. Lancet Psychiatry. 2020 Oct;7(10):883-892. doi: 10.1016/S2215-0366(20)30308-4. Epub 2020 Jul 21. PMID: 32707037; Link to PubMed
Proto E. et al.
Proto E, Quintana-Domeque C. COVID-19 and mental health deterioration by ethnicity and gender in the UK. PLoS One. 2021 Jan 6;16(1):e0244419. doi: 10.1371/journal.pone.0244419. Link to PubMed
Ramiz L. et al.
Ramiz L, Contrand B, Rojas Castro MY, Dupuy M, Lu L, Sztal-Kutas C, Lagarde E. A longitudinal study of mental health before and during COVID-19 lockdown in the French population. Global Health. 2021 Mar 22;17(1):29. doi: 10.1186/s12992-021-00682-8. PMID: 33752717; PMCID: PMC7982911. Link to PubMed
Sibley CG. et al.
Sibley CG, Greaves LM, Satherley N, Wilson MS, Overall NC, Lee CHJ, Milojev P, Bulbulia J, Osborne D, Milfont TL, Houkamau CA, Duck IM, Vickers-Jones R, Barlow FK. Effects of the COVID-19 pandemic and nationwide lockdown on trust, attitudes toward government, and well-being. Am Psychol. 2020 Jul-Aug;75(5):618-630. doi: 10.1037/amp0000662. Epub 2020 Jun 4. PMID: 32496074. Link to PubMed
Teng Z et al.
Teng Z, Pontes HM, Nie Q, Griffiths MD, Guo C. Depression and anxiety symptoms associated with internet gaming disorder before and during the COVID-19 pandemic: A longitudinal study. J Behav Addict. 2021 Mar 10. doi: 10.1556/2006.2021.00016. Epub ahead of print. PMID: 33704085. Link to Pubmed
van der Velden PG. et al. 1
van der Velden PG, Contino C, Das M, van Loon P, Bosmans MWG. Anxiety and depression symptoms, and lack of emotional support among the general population before and during the COVID-19 pandemic. A prospective national study on prevalence and risk factors. J Affect Disord. 2020;277:540-548. doi:10.1016/j.jad.2020.08.026 Link to PubMed
van der Velden PG. et al. 2
van der Velden PG, Hyland P, Contino C, von Gaudecker HM, Muffels R, Das M. Anxiety and depression symptoms, the recovery from symptoms, and loneliness before and after the COVID-19 outbreak among the general population: Findings from a Dutch population-based longitudinal study. PLoS One. 2021 Jan 7;16(1):e0245057. doi: 10.1371/journal.pone.0245057. Link to PubMed



